If you are reading this, chances are you or someone you has been looking for lasting back pain relief. It’s human nature to want to know the cause of the pain. For many, this leads to getting some x-rays. That’s good. If the pain is difficult to explain, getting these images are important to rule out some scarier diagnosis. The issue however is when the results come back with “degenerative disc disease” or “disc bulge”. In my years of clinical practice, I have seen how strongly patients hold onto these diagnostic terms. Even more concerning is how we interpret what disc pathologies mean. For many the immediate assumption is that their spine is frail, that their discs are crumbling and more importantly, are unable to heal beyond invasive medical procedures such as PRP injection or surgery.
As a physiotherapist and educator, I want to collaborate with you to change this narrative. Some of the apprehension patients feel arises simply from the word “degeneration,” making it incredibly worthwhile to differentiate what this actually means. It is time to move away from the outdated degenerative narrative and embrace your spine’s incredible adaptive potential.
Let’s dive into the science of intervertebral disc health and explore how you can actively build a stronger, more resilient back.
The Science: Why You Aren't a "Jelly Donut"
For decades, the medical field used a flawed metaphor to describe spinal discs: the “jelly donut.” While it is true that the disc is comprised of two parts; a thick outer area (annulus fibrosis) and a softer inner layer (nucleus pulposus), the analogy of a leaking jelly donut can lead a person to think this structure is fragile. In reality the disc is incredibly resilient, absorbing forces many times greater than their body weight without damage.
We aren’t ignoring that disc bulges happen. In fact, the vast majority of people will experience a disc bulge over their lifetime. One study reported that disk bulges are range from 30% of 20 year olds and increasing to 84% of those 80 years of age (1). What needs to be emphasized though is that when a disc bulge happens, it’s not a slow leak of jam out into your spine. It is controlled and slowly cleaned up by your body. Like any tissue in your body, the disc is capable of repair, and even more importantly, capable of adaptation. The key here is the environment. If the disc exists in an environment of disuse and without nutrients, it will become less healthy (degenerate). Conversely, if the disc is placed in the right environment, it will become more resilient.
An issue here is how we often see the word degenerate. It is easy to view degenerations as a slow, inevitable breakdown of a tissue. When we talk about disc degeneration, from a physiological perspective, we are speaking of reduced disc height, reduced hydration and increased fibrous tissues (2).
The good news is that some of these features of disc degeneration are reversible. Your intervertebral discs are not static shock absorbers; they are dynamic, living tissues highly responsive to their environment.
Instead of a jelly donut, think of your disc like a sponge in a bucket of water.


Spinal discs lack a direct blood supply. Nutrient exchange—the delivery of oxygen, water, and vital ions—is entirely dependent on mechanical loading. When you walk, jog, or lift, you compress and decompress the disc. You are essentially squeezing the dirty water out of the sponge and allowing it to soak up fresh, nutrient-rich fluid. As you repeated compress and the decompress the disc, there are positive improvements in disc metabolism and health (3).
In fact, inactivity starves the disc. Extended sedentary behaviour leads to reduced oxygen diffusion and increased acidity. Over time, this creates an environment where normal age-related changes can become sensitized and painful (4). Conversely, human and animal research consistently shows that dynamic activities like running and walking lead to anabolic adaptation, meaning the disc physically adapts to become thicker and stronger over time.
Are you letting back pain keep you from the activities you love? Don’t let a sensitive back turn into a chronic issue. Book a comprehensive back assessment with our Victoria team today.
What the Research Actually Says About Exercise and Spinal Health
To truly practice evidence-based care, we have to look at the highest quality data available. A comprehensive review was conducted with the specific study aim to determine whether exercise training, sport participation, and physical activity improve continuous measures of disc health, compared with controls who do not participate in the same physical loading (5).
The review looked at all humans and measured the exposure of physical activity via exercise training, sport participation, or general physical activity. The studies compared those engaging in more exercise active groups against inactive or non-participating control groups to see if there would be changes in the disc health.
The primary analysis found a small effect of better disc health in those engaging in physical activity compared to the control group (hopefully, no surprise here).
But if we dig into the data a bit more, things get interesting:
- Upright bipedal physical loading (such as walking,running, skiing, etc) resulted in significantly better disc health compared to any other exercise group
- Conversely, explosive activities like weightlifting, martial arts, and baseball had a negligible difference in IVD health
The takeaway form this is that we should be using low intensity repetitive exercise to promote effective “circulation” in our discs. While weightlifting didn’t improve disc health, it also didn’t make it worse. There are many benefits to weight lifting outside disc health; significantly improving your muscular and bone health, so we shouldn’t throw it out of your training program!
The Framework: How We Build Disc Resiliency for lasting Back Pain Relief
At Pursuit Physiotherapy, we don’t just aim to temporarily manage symptoms; we focus on progressive desensitization and long-term robustness. We use a structured approach to guide your recovery:
1. Find the “Anabolic Window”
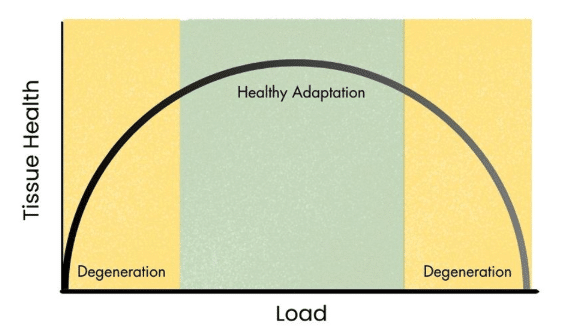
There is a sweet spot for tissue adaptation. Research shows a U-shaped relationship with disc health: poorer health is seen at the extreme ends of the spectrum (highly sedentary individuals versus those exposed to unmanaged, explosive physical loading). Our goal is to find your specific anabolic window—the moderate dynamic loading that elicits positive structural changes without overwhelming your current capacity.

2. Motion is Lotion
Your discs love load. We aren’t asking people to repeatedly deadlift here (we love deadlifts, and they are great for discs and back health, just not the only way to do this!). What we are asking is that people move their bodies throughout the day incorporating some sort of repeated low back bending or with mild impact (such as in walking) to facilitate this pumping mechanism in the disc. With increasing access to technology and office work, we are seeing a rise in sedentary behaviour across the globe. This sedentary behavior may directly contribute to or increase the risk for progressive disc degeneration. The research is highly compelling: in one study spanning over 14 years, individuals exercising for less than an hour a day had more rapid lumbar disc narrowing and signal loss compared to those exercising for more than 2 hours (6). Put into action, this means incorporating a 20 minute walk each day, something we can all find a way to fit in.
3. Progressive Desensitization
When your back is highly irritable or in a protective muscle spasm, our first goal is to calm the nervous system. We might use targeted manual therapy or recommend specific acute back pain strategies to manage symptoms.
Once the system is calm, we build it up. We introduce isolated lumbar extensor exercises and functional strength training. Even heavy resistance training, when dosed correctly and progressed safely by a qualified professional, produces substantial, healthy lumbar loading that tells your body to build a more robust spine. This process is variable, for some they are able to progress quickly and for others it is slower. The factors playing into this process are complex including beliefs, general health, lifestyle, and chronicity of pain. The good news is that with so many elements factoring into a person’s pain, there are many ways to approach and resolve the issue!
Your Next Steps to a Robust Spine
Pain is an incredibly complex experience, but it does not mean your body is broken. The belief that your spine is fragile is one of the biggest barriers to recovery. We see incredible, spontaneous adaptations in the clinic every day. Recent robust meta-analyses have even shown that a large majority of significant disc issues spontaneously resolve and heal on their own when given the right environment.
You don’t have to stop hiking Mt. Doug or give up your spot in the TC10K because of a sensitive back. You just need a roadmap to rebuild your tolerance.
Ready to build a more resilient body? Let’s find your starting point. Book an assessment at Pursuit Physiotherapy today.
Key References:
- Brinjikji W, Luetmer PH, Comstock B, et al. Systematic literature review of imaging features of spinal degeneration in asymptomatic populations. AJNR Am J Neuroradiol. 2015;36(4):811-816. doi:10.3174/ajnr.A4173
- Brinjikji W, Diehn FE, Jarvik JG, et al. MRI findings of disc degeneration are more prevalent in adults with low back pain than in asymptomatic controls: a systematic review and meta- analysis. Am J Neuroradiol. 2015;36(12):2394–9.
- Chan SC, Ferguson SJ, Gantenbein-Ritter B. The effects of dynamic loading on the intervertebral disc. Eur Spine J. 2011;20(11):1796-1812. doi:10.1007/s00586-011-1827-1
- Steele J, Bruce-Low S, Smith D, Osborne N, Thorkeldsen A. Can specific loading through exercise impart healing or regeneration of the intervertebral disc?. Spine J. 2015;15(10):2117-2121. doi:10.1016/j.spinee.2014.08.446
- Samanna CL, Owen PJ, Mitchell UH, et al. The Impact of Exercise on Intervertebral Disc Health: A Systematic Review and Meta-Analysis. Sports Med. Published online March 16, 2026. doi:10.1007/s40279-025-02336-w
- Maurer E, Klinger C, Lorbeer R, et al. Long-term effect of physical inactivity on thoracic and lumbar disc degeneration-an MRI-based analysis of 385 individuals from the general population. Spine J. 2020;20(9):1386-1396. doi:10.1016/j.spinee.2020.04.016
Disclaimer: The content provided here is for educational purposes only and does not constitute medical advice. Every injury is unique. For a specific diagnosis and treatment plan, please book an appointment with our team.




